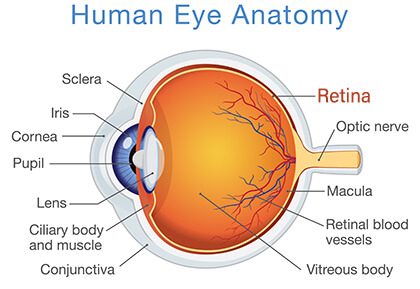
What is the retina?
The retina is a thin membrane on the back of the eye that is lined with photoreceptor cells. These light-sensitive cells function to process light and convert it into neural signals that are sent to the brain for visual recognition.
Why is the retina important?
The retina plays a critical role in vision — if it is damaged, the brain won’t be able to receive visual information, which can result in permanent blindness. Often, the first signs of damage are hard to notice. By the time you notice a decrease in vision quality, the damage is irreversible.
It’s very important to monitor your eye health so retinal conditions can be detected and treated as early as possible. The best way to evaluate retinal health is to schedule regular exams with an eye care professional. If a retinal condition is caught early, your doctor can develop a treatment plan to prolong your vision.
What are common retinal conditions?
There are many conditions that can affect your retina, but some are more common than others.
Here are the eye conditions most likely to cause retinal damage:
– Diabetic Retinopathy: Symptoms of uncontrolled diabetes can affect your retinal health. High blood sugar levels can cause the blood vessels in the retina to swell. When the vessels swell too much, they can start to leak and cause damage to the retina.
– Macular Degeneration: Age-Related Macular Degeneration is one of the most common retinal conditions. It occurs when the photoreceptor cells in the macula — the center of the retina — begin to break down. As a result, central vision begins to fade.
– Retinal Tear or Detachment: The vitreous, a gel that fills most of the eye, can sometimes shrink and pull the retina with it. This can result in a retinal tear or a complete detachment. When this happens, the symptoms are often immediate and include the sudden appearance of floaters in your field of vision. If you experience a tear or detachment, you should seek treatment immediately, as they are considered a medical emergency. If not immediately treated, a detachment can cause permanent blindness.
How do you maintain a healthy retina?
One of the best ways to maintain a healthy retina is to have good health in general. An active lifestyle and proper nutrition can help lower your risk of retinal disease, in addition to staying consistent with routine eye examinations. Since retinal damage is irreversible by the time your vision declines, early detection and treatment is the best way to prevent vision loss.
What happens during a retinal exam?
Most regular eye exams include a retinal exam. A comprehensive eye exam may include a detailed retinal scan using Ocular Coherence Tomography (OCT). This test uses infrared technology to provide detailed images of the retina, which are typically better for detecting early stage retinal damage. Your doctor will recommend the tests that are right for you.
How often should you have an eye exam?
Adults ages 18-55 should schedule a comprehensive eye exam at least once every two years to check for changes in vision and to assess for a variety of eye conditions. Annual exams are recommended for adults over age 55 and individuals who are considered “at risk.” In addition to age, risk factors include eye injuries, complications from a surgery, diabetes, or a family history of eye disease.
If you experience problems with your vision, consult your eye doctor as soon as possible — don’t wait until your scheduled appointment. A sudden change in your eyesight could indicate a serious problem that requires immediate attention. Contact emergency services if your eye doctor isn’t available.
How do you treat a retinal condition?
There are a variety of treatment options for retinal damage. Treatment is typically most effective when used as early as possible to prevent further damage.
These treatments include:
– Anti-VEGF Injections: Certain medications can be injected into the eye in order to stop the growth of abnormal blood vessels as a result of diabetic retinopathy. Anti-VEGF medications target the Vascular endothelial growth factor, or VEGF, which is a type of protein that causes abnormal vessel growth in patients with diabetic retinopathy.
– Vitrectomy: The vitreous can cause issues when it pulls on the retina. A vitrectomy removes the gel-like substance and replaces it with an oilier substance that reduces the amount of tension it has on the retina.
– Focal or Scatter Laser Photocoagulation: One of the most common surgical methods used to treat diabetic retinopathy is laser surgery. Either a focused laser or a scattered laser is used to seal off leaking blood vessels in the retina, which causes the abnormal blood vessels to shrink and minimize damage.




No more posts